Percutaneous Transhepatic Biliary Drainage & Stenting (PTBD)
A Minimally Invasive Way to Relieve Bile Duct Blockage and Jaundice
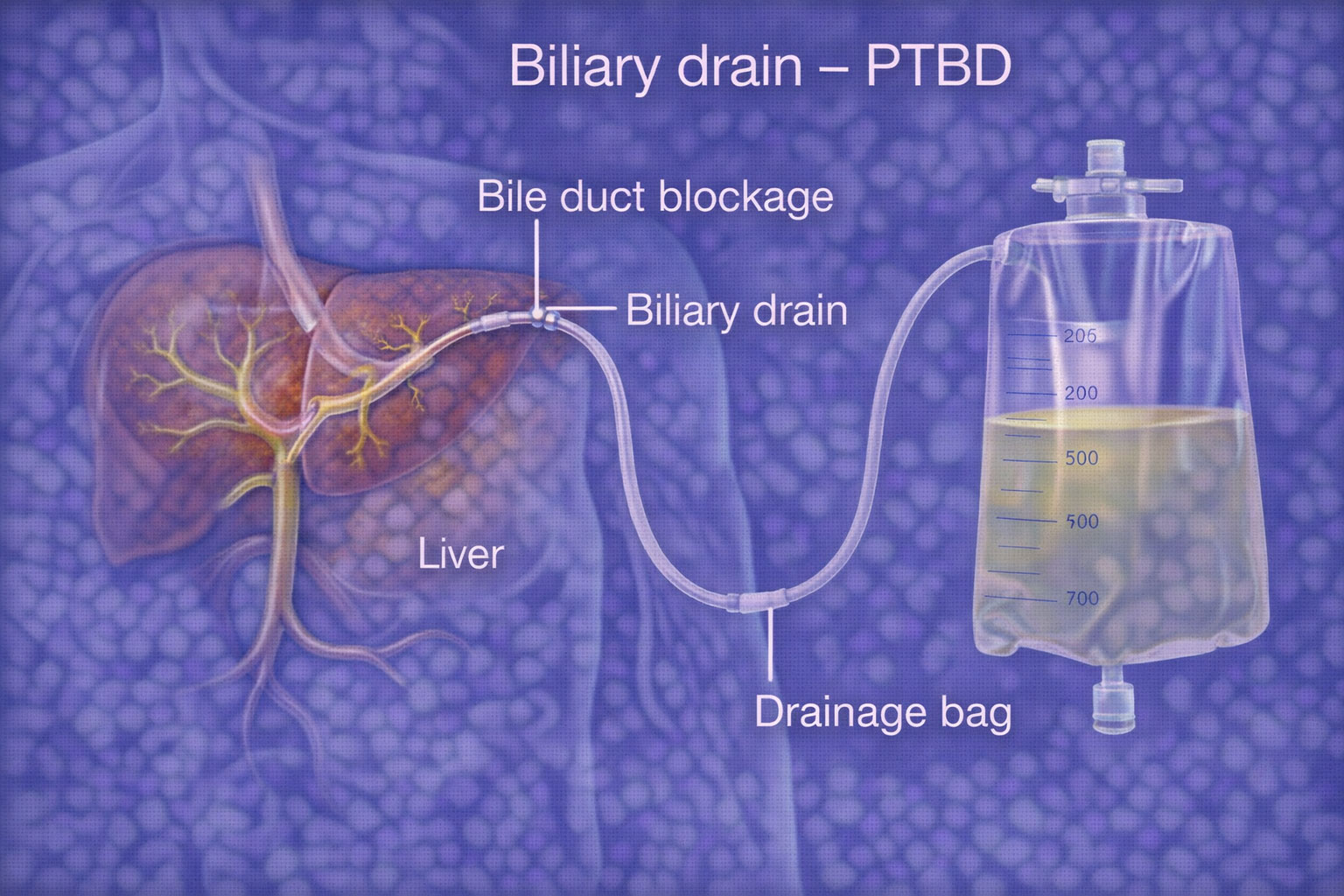
When the bile ducts get blocked, bile cannot flow from the liver to the intestine. This can cause jaundice (yellow eyes/skin), itching, infection, pain, and liver damage.
Percutaneous Transhepatic Biliary Drainage & Stenting (PTBD) is a minimally invasive, image-guided procedure that drains bile and/or places a stent to open the blocked bile duct, giving quick relief from jaundice and infection—often without major surgery.