A Minimally Invasive Way to Treat Abnormal Brain Blood Vessels and Reduce Bleeding Risk
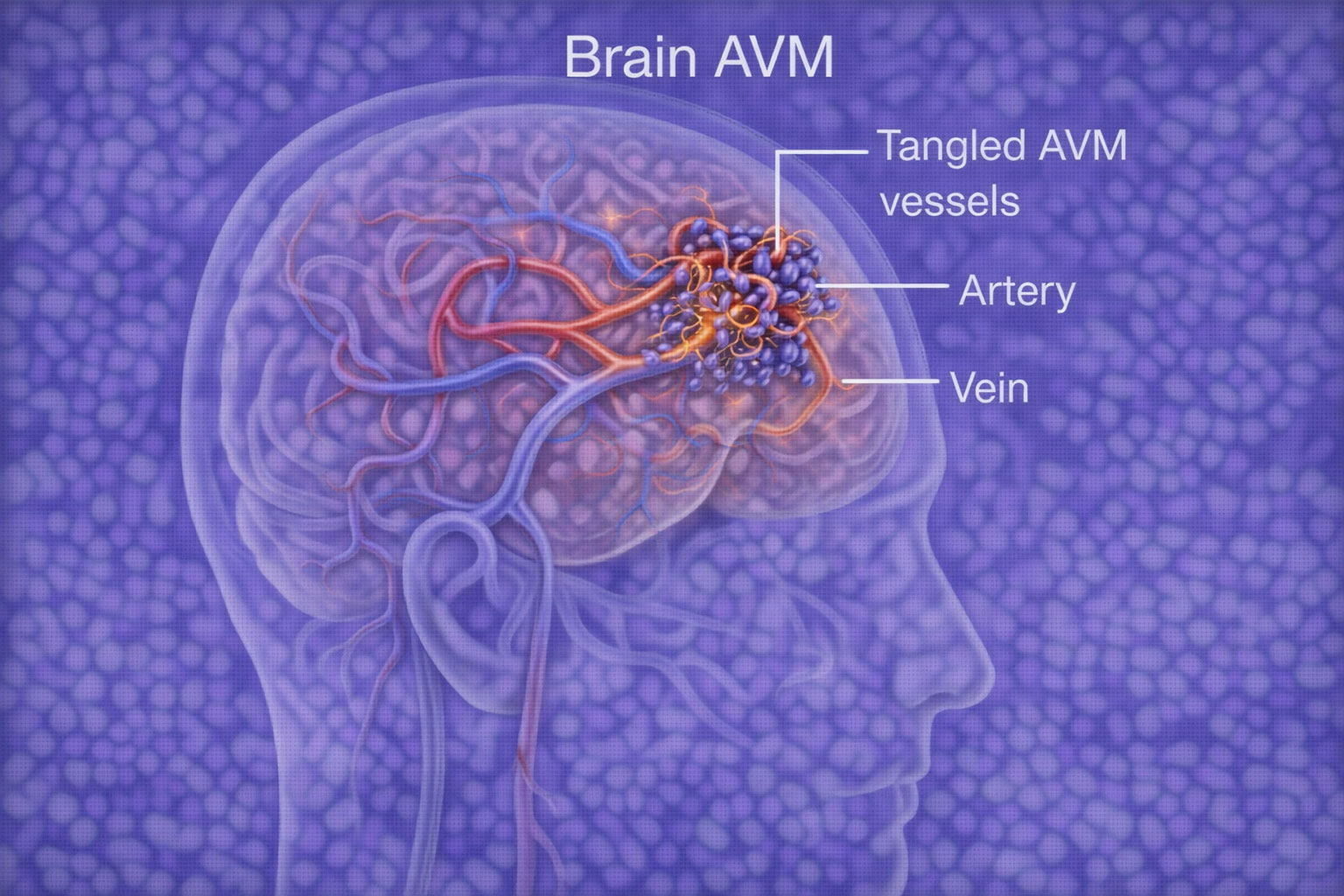
A Brain AVM (Arteriovenous Malformation) is an abnormal tangle of blood vessels in the brain that can bleed suddenly and cause stroke, seizures, or brain damage.
Brain AVM embolization is a modern, minimally invasive treatment that blocks the abnormal blood vessels from inside, helping to reduce the risk of bleeding and often make surgery or radiation safer and more effective.