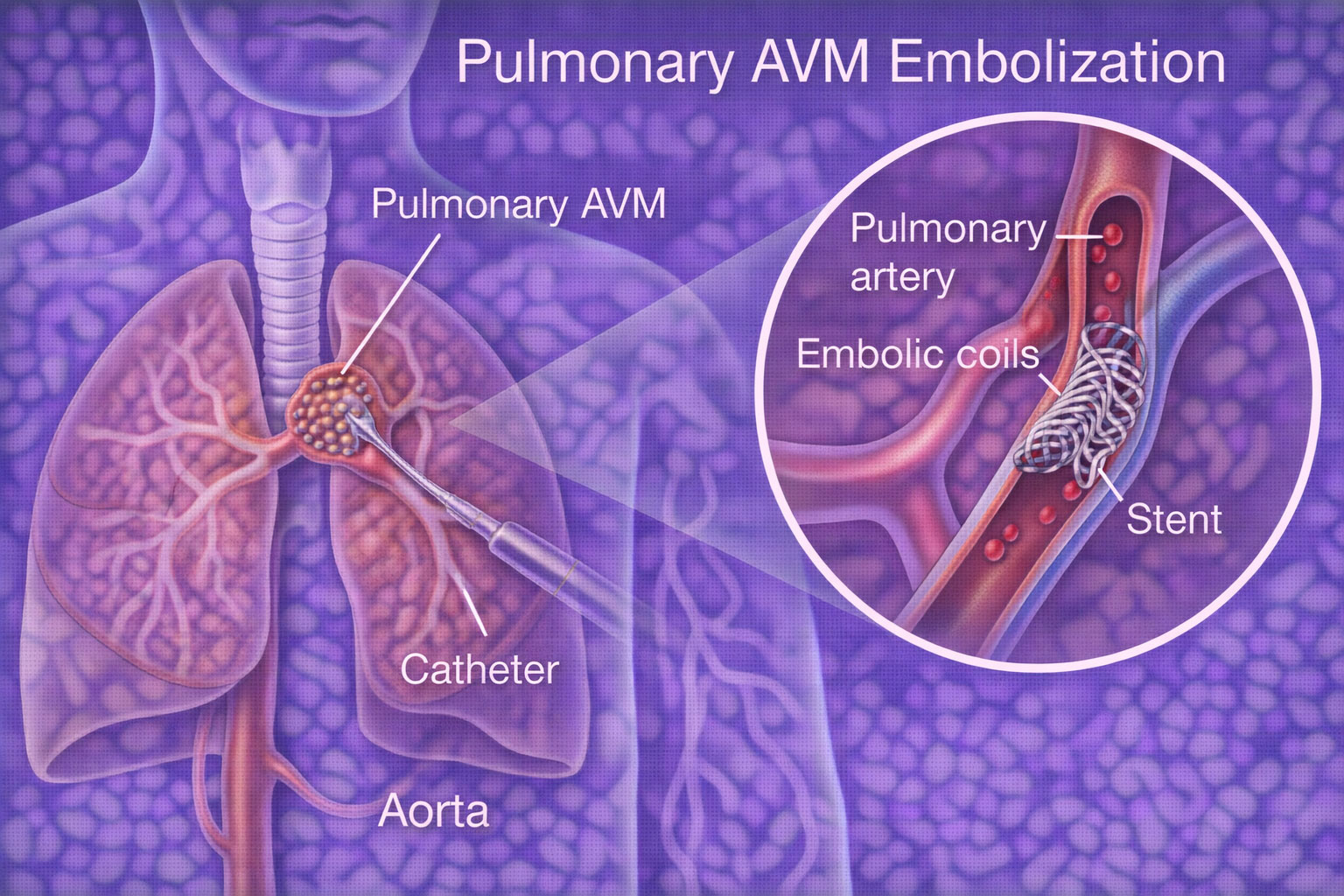
A Safe, Minimally Invasive Treatment to Prevent Stroke and Bleeding from Lung AVMs
A Pulmonary AVM (Arteriovenous Malformation) is an abnormal connection between an artery and a vein in the lungs. This allows blood to bypass the normal filtering system of the lungs, which can lead to breathlessness, low oxygen levels, stroke, brain abscess, or bleeding.
Pulmonary AVM embolization is a minimally invasive, image-guided procedure that blocks this abnormal connection from inside the blood vessel—often without surgery—and protects you from serious complications.